Flipping Out About Flip Flops
Although it may be tempting to wear flip-flops in warm weather, they are not the best choice of footwear for your feet. Flip-flops may be ideal for the beach, pool, spa, and shared showers, but you should avoid wearing them unless it is completely necessary.
Flip-flops only have a small strip of fabric holding your foot in place, but your toes need a better grip to keep your foot in place. The repetitive gripping can lead to an overuse of your muscles, which could result in tendinitis. This is only one of the many problems that stem from wearing flip-flops too often.
Flip flops aren’t good for extensive walking because they fail to offer arch support, heel cushioning, or shock absorption. As a result, people who wear flip flops are at a higher risk of experiencing an ankle sprain. Additionally, these shoes offer little protection for your feet, putting those who wear them at a greater risk for stubbed toes, glass cuts, and puncture wounds.
Although flip flops aren’t recommended for everyday use by anyone, it is especially important for diabetics to avoid them. A diabetic foot injury can easily become very serious, and it may even lead to amputation.
If you are experiencing pain from wearing flip-flops, you shouldn’t be hesitant to replace them with a more comfortable shoe that offers more support. If your flip-flop foot pain doesn’t go away, you should seek assistance from a podiatrist right away. It is possible that you may have a more serious foot problem such as a stress fracture or arthritis.
Risk Factors for Falling

As people age, the risk of a fall increases, but it should not be seen as inevitable. Falls can be caused by various factors, including weak muscles, poor balance, and dizziness. Foot problems like pain or deformities, and cognitive issues such as memory loss, and vision and hearing impairments, can also contribute to the risk of falls in seniors. Medications that induce drowsiness, excessive alcohol consumption, and certain bladder or bowel conditions can increase the likelihood of falling. Falls often result from an interaction of these factors, with a higher number of risk factors further elevating the potential for falls. In addition, falls can sometimes signal underlying health issues like constipation, infections, dehydration, or sudden confusion. A podiatrist can provide expert advice and interventions to address foot-related problems, improve balance, and reduce the risk of future falls. If instability causes you to lose your balance or fall frequently, it is suggested that you schedule an appointment with a podiatrist for a thorough exam and options for treatment.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Milos Tomich, DPM from Dr. Tomich Foot & Ankle Health Center. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact one of our offices located in Milwaukee and Wauwatosa, WI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Falls Prevention
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
How Shoe Choice Can Cause Hind-Foot Pain
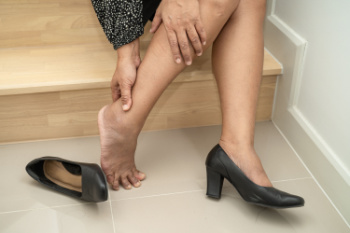 Wearing improper footwear, particularly shoes that lack adequate support or fit poorly, can significantly contribute to hind-foot pain. High heels and narrow-toed shoes, while fashionable, can place excessive stress on the structures of the hind-foot. The heel and ankle are two particularly susceptible areas for pain. Wearing these kinds of shoes can also lead to conditions like plantar fasciitis, Achilles tendonitis, and bursitis. These styles force the foot into an unnatural position, disrupting alignment and increasing pressure on the back of the foot. Stress on the foot over time not only leads to pain and discomfort but also can significantly affect mobility and quality of life. It is important to choose shoes with proper support, cushioning, and a fit that accommodates the natural shape of the foot to prevent hind-foot pain. Podiatrists often stress the importance of wearing shoes that complement one's lifestyle as well as provide the foundation for healthy foot posture and function. If you are experiencing pain in the back of the foot, it is suggested that you visit a podiatrist for a full diagnosis and proper shoe recommendations to support your recovery.
Wearing improper footwear, particularly shoes that lack adequate support or fit poorly, can significantly contribute to hind-foot pain. High heels and narrow-toed shoes, while fashionable, can place excessive stress on the structures of the hind-foot. The heel and ankle are two particularly susceptible areas for pain. Wearing these kinds of shoes can also lead to conditions like plantar fasciitis, Achilles tendonitis, and bursitis. These styles force the foot into an unnatural position, disrupting alignment and increasing pressure on the back of the foot. Stress on the foot over time not only leads to pain and discomfort but also can significantly affect mobility and quality of life. It is important to choose shoes with proper support, cushioning, and a fit that accommodates the natural shape of the foot to prevent hind-foot pain. Podiatrists often stress the importance of wearing shoes that complement one's lifestyle as well as provide the foundation for healthy foot posture and function. If you are experiencing pain in the back of the foot, it is suggested that you visit a podiatrist for a full diagnosis and proper shoe recommendations to support your recovery.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Milos Tomich, DPM from Dr. Tomich Foot & Ankle Health Center. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact one of our offices located in Milwaukee and Wauwatosa, WI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Pain
The feet, being the foundation of the body, carry all of the body’s weight and are therefore prone to experiencing pain and discomfort. If you are experiencing foot pain, it is important to determine where in the foot you are experiencing this pain to help discover the cause of it. While pain can be experienced virtually anywhere in the foot, the most common sites of foot pain are in the heel and ankle.
Heel pain can be due to a multitude of conditions including plantar fasciitis, Achilles tendinitis, and heel spurs. Pain experienced in the ankle can be a sign of an ankle sprain, arthritis, gout, ankle instability, ankle fracture, or nerve compression. In more serious cases, pain in the foot can be a sign of improper alignment or an infection.
Foot pain can be accompanied by symptoms including redness, swelling, stiffness and warmth in the affected area. Whether the pain can be described as sharp or dull depends on the foot condition behind it. It is important to visit your local podiatrist if your foot pain and its accompanying symptoms persist and do not improve over time.
Depending on the location and condition of your foot pain, your podiatrist may prescribe certain treatments. These treatments can include but are not limited to prescription or over-the-counter drugs and medications, certain therapies, cortisone injections, or surgery.
If you are experiencing persistent foot pain, it is important to consult with your foot and ankle doctor to determine the cause and location. He or she will then prescribe the best treatment for you. While milder cases of foot pain may respond well to rest and at-home treatments, more serious cases may take some time to fully recover.
Ankle Joint Replacement Surgery for Arthritis Relief
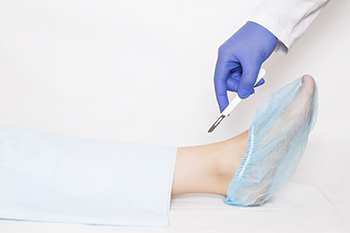 Joint replacement for ankle arthritis is a surgical option for those suffering from severe arthritis in their ankle. The point of the replacement surgery is to relieve pain and restore the function of the ankle. Arthritis is characterized by the breakdown of cartilage that cushions the ends of the bones, leading to pain, stiffness, and reduced mobility. During ankle joint replacement surgery, also known as ankle arthroplasty, the damaged parts of the ankle bones are removed and replaced with artificial components. These components mimic the natural movement of the ankle, offering patients the chance to regain mobility. This procedure is considered when less invasive treatments have failed to provide relief. It is also considered mostly for older, less active patients. Joint replacement can significantly reduce pain and improve the ankle's function, making it a valuable treatment option for those with advanced ankle arthritis. If you are suffering from arthritis in the ankle, it is suggested that you schedule an appointment with a podiatrist to discuss whether ankle replacement surgery is right for you.
Joint replacement for ankle arthritis is a surgical option for those suffering from severe arthritis in their ankle. The point of the replacement surgery is to relieve pain and restore the function of the ankle. Arthritis is characterized by the breakdown of cartilage that cushions the ends of the bones, leading to pain, stiffness, and reduced mobility. During ankle joint replacement surgery, also known as ankle arthroplasty, the damaged parts of the ankle bones are removed and replaced with artificial components. These components mimic the natural movement of the ankle, offering patients the chance to regain mobility. This procedure is considered when less invasive treatments have failed to provide relief. It is also considered mostly for older, less active patients. Joint replacement can significantly reduce pain and improve the ankle's function, making it a valuable treatment option for those with advanced ankle arthritis. If you are suffering from arthritis in the ankle, it is suggested that you schedule an appointment with a podiatrist to discuss whether ankle replacement surgery is right for you.
In certain cases, in which the patient suffers from extreme pain or damage in a joint, joint replacement surgery may be deemed useful. If you have constant pain in a foot joint, consult with Milos Tomich, DPM from Dr. Tomich Foot & Ankle Health Center. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Joint Replacement Surgery?
Over time, joints wear down; this can be exacerbated by diseases and conditions. Joint replacement surgery, also known as arthroplasty, is when a damaged joint is surgically removed and replaced with a prosthesis. Prostheses, which can be made of ceramic, plastic, or metal, act as joints in lieu of an actual joint. One of the most prevalent causes for joint replacement is arthritis.
Arthritis in the Foot
Arthritis can occur in any joint in the body, including in the feet. Common types of arthritis in the foot are osteoarthritis, rheumatoid arthritis, and gout. The big toe is usually where arthritis occurs in the foot; this is known as hallux rigidus.
Joint Replacement Surgery in the Foot
The most common form of joint replacement in the foot is a first metatarsophalangeal (MTP) joint placement. MTP joint replacement surgery is designed to treat hallux rigidus. Surgery is not intensive, and recovery occurs within one to two months after the procedure has been done. Overall, joint replacement surgery is a safe and effective way to treat pain in the joint of the foot.
If you have any questions, please feel free to contact one of our offices located in Milwaukee and Wauwatosa, WI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Joint Replacement Surgery
When conservative, noninvasive treatments prove unsuccessful, podiatrists will often turn to surgery as the last line of treatment for their patients. If patients are suffering from joint pain, issues in mobility, or are seeking to correct a deformity, joint replacement surgery is an effective option. Joint replacement surgery is also successful in treating arthritis, which is the most common cause of improperly working joints.
Patients with symptoms that include joint pain, stiffness, limping, muscle weakness, limited motion, and swelling are typically considered for joint replacement surgery. Range of motion and activity post-surgery will vary between patients and depending on the specific surgery performed, the affected joint, and the damage that will need to be repaired.
Joint replacement surgery replaces the damaged cartilage and bone, the latter if required. The damaged cartilage is typically replaced with a prosthesis that is attached to the bone, allowing the implant to grow into the bone. Following surgery, the patient will typically undergo physical therapy to become familiar with movement using the replaced joint.
Conditions Associated With Heel Spurs
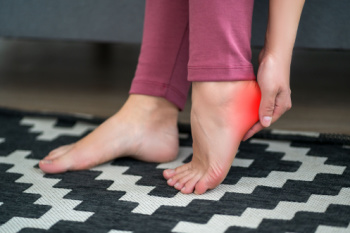 Heel spurs are bony growths that develop on the underside of the heel bone, often near the point where the plantar fascia connects to the bone. While they can be asymptomatic, heel spurs are frequently associated with certain foot conditions, serving as indicators of underlying issues. Primarily, they're linked with plantar fasciitis, a condition where the ligament running along the bottom of your foot becomes inflamed and causes heel pain. This inflammation can lead to the development of a spur. Heel spurs are also frequently associated with chronic conditions stemming from strain on the foot muscles and ligaments, or from repeated tearing of the membrane that covers the heel bone. Such strain and tearing can be due to excessive weight, poor shoe choices, or an active lifestyle without adequate foot support. The association of heel spurs with other conditions typically means there will be a comprehensive approach to treatment, which may include stretches, orthotic support, or lifestyle modifications to address the root cause of the pain. If you are suffering from a heel spur, it is suggested you make an appointment with a podiatrist who can diagnose the underlying problem and help you find relief.
Heel spurs are bony growths that develop on the underside of the heel bone, often near the point where the plantar fascia connects to the bone. While they can be asymptomatic, heel spurs are frequently associated with certain foot conditions, serving as indicators of underlying issues. Primarily, they're linked with plantar fasciitis, a condition where the ligament running along the bottom of your foot becomes inflamed and causes heel pain. This inflammation can lead to the development of a spur. Heel spurs are also frequently associated with chronic conditions stemming from strain on the foot muscles and ligaments, or from repeated tearing of the membrane that covers the heel bone. Such strain and tearing can be due to excessive weight, poor shoe choices, or an active lifestyle without adequate foot support. The association of heel spurs with other conditions typically means there will be a comprehensive approach to treatment, which may include stretches, orthotic support, or lifestyle modifications to address the root cause of the pain. If you are suffering from a heel spur, it is suggested you make an appointment with a podiatrist who can diagnose the underlying problem and help you find relief.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact Milos Tomich, DPM from Dr. Tomich Foot & Ankle Health Center. Our doctor will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main condition's spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions feel free to contact one of our offices located in Milwaukee and Wauwatosa, WI . We offer the latest in diagnostic and treatment technology to meet your needs.
Heel Spurs
Heel spurs are the result of calcium deposits that cause bony protrusions on the underside of the heel. Heel spurs are usually painless, but they have the potential to cause heel pain. Heel spurs tend to be associated with plantar fasciitis, which is a condition that causes inflammation of the band of connective tissue that runs along the bottom of the foot. They most often occur to athletes whose sports involve a lot of running and jumping.
Some risk factors for developing heel spurs include running and jogging on hard surfaces, being obese, wearing poorly fitting shoes, or having walking gait abnormalities.
It is possible to have a heel spur without showing signs of any symptoms. However, if inflammation develops at the point of the spur’s formation, you may have pain while walking or running. In terms of diagnosis, sometimes all a doctor needs to know is that the patient is experiencing a sharp pain localized to the heel to diagnose a heel spur. Other times, an x-ray may be needed to confirm the presence of a heel spur.
Heel spurs can be prevented by wearing well-fitting shoes that have shock-absorbent soles. You should also be sure that you are choosing the right shoe for the activity you want to partake in; for example, do not wear walking shoes when you want to go on a run. Additionally, maintaining a healthy weight can be beneficial toward preventing heel spurs, as it will prevent an excess amount of pressure being placed on the ligaments.
There are a variety of treatment options for people with heel spurs. Some of these include stretching exercises, physical therapy, shoe inserts, or taping and strapping to rest stressed muscles and tendons. If you have heel pain that lasts longer than a month, don’t hesitate to seek help from a podiatrist. Your doctor can help you determine which treatment option is best for you.