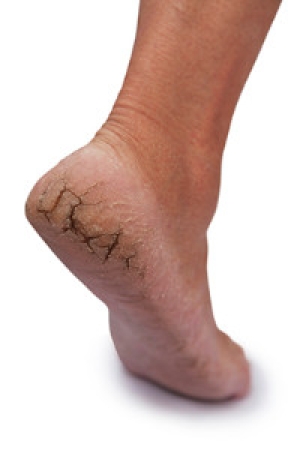
What Are The Symptoms Of Tarsal Tunnel Syndrome?
 If the nerves are affected in the ankle, foot and toes, you may have a condition that is known as tarsal tunnel syndrome. Some of the symptoms that are associated with this ailment can include numbness, or a burning and tingling sensation. If an injury has occurred, and the tissues surrounding the tibial nerve become inflamed, this condition may develop. The pain and discomfort is typically felt in the heel and may extend to the sole of the foot. There are a number of reasons why this ailment can occur. These often include stress fractures, being overweight, or having flat feet. There may be existing conditions that put pressure on the nerves within the tarsal tunnel, and this may cause inflammation to occur. If you have any of the symptoms that have been mentioned, it is suggested to speak to a podiatrist who can guide you toward proper treatment options.
If the nerves are affected in the ankle, foot and toes, you may have a condition that is known as tarsal tunnel syndrome. Some of the symptoms that are associated with this ailment can include numbness, or a burning and tingling sensation. If an injury has occurred, and the tissues surrounding the tibial nerve become inflamed, this condition may develop. The pain and discomfort is typically felt in the heel and may extend to the sole of the foot. There are a number of reasons why this ailment can occur. These often include stress fractures, being overweight, or having flat feet. There may be existing conditions that put pressure on the nerves within the tarsal tunnel, and this may cause inflammation to occur. If you have any of the symptoms that have been mentioned, it is suggested to speak to a podiatrist who can guide you toward proper treatment options.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact Milos Tomich, DPM of Dr. Tomich Foot & Ankle Health Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact one of our offices located in Milwaukee and Wauwatosa, WI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome is a condition in which there is a compression of the posterior tibial nerve. The posterior tibial nerve runs along the inside of the ankle into the foot. Tarsal tunnel syndrome is named for the tarsal tunnel, which is a thin space along the inside of the ankle beside the ankle bones. This space contains various nerves, arteries, and tendons, and includes the posterior tibial nerve. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome the tibial nerve is compressed, causing tingling or burning, numbness, and pain.
Common causes of tarsal tunnel syndrome involve pressure or an injury. Injuries that produce inflammation and swelling in or around the tunnel may place pressure on the posterior tibial nerve. Direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or trauma to the tibial nerve, can result in tarsal tunnel syndrome. Diseases that damage nerves, such as diabetes or arthritis, may cause tarsal tunnel syndrome. Those with flat feet are at risk for developing the condition, as the extra pressure and strain placed on the foot may compress the posterior tibial nerve.
Feeling different sensations in the foot at different times is a common symptom of tarsal tunnel syndrome. An afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg. Symptoms are primarily felt on bottom of the foot and/or the inside of the ankle. Symptoms can appear suddenly and may occur due to overuse of the foot.
To diagnose tarsal tunnel syndrome, your podiatrist may examine the foot and tap the posterior tibial nerve to see if symptoms surface. He or she may also order an MRI to determine if a mass is present.
Treating tarsal tunnel syndrome will depend on the decision of your podiatrist. Multiple options are available, however, and can include rest, ice, immobilization, oral medications such as anti-inflammatory drugs (NSAIDS), physical therapy, injection therapy, orthotics, supportive shoes, braces, and surgery.
Foot Ulcers and Diabetes
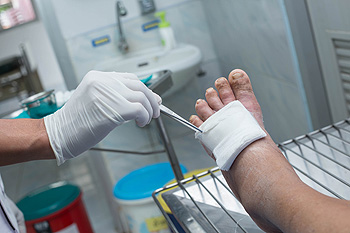 Patients with diabetes are often familiar with foot conditions that can develop as a result of this affliction. Research has indicated the importance of having regular foot examinations, as this can be helpful in noticing any cuts or wounds that have developed on the feet. Diabetes can produce tingling and numbing sensations in the feet. This may cause difficulty in feeling any cuts that are present on the feet, which can lead to infections. If the cuts are not properly cared for, foot ulcers may develop and gangrene may gradually develop. If you have diabetes, it is advised that you be under the care of a podiatrist who can manage this condition.
Patients with diabetes are often familiar with foot conditions that can develop as a result of this affliction. Research has indicated the importance of having regular foot examinations, as this can be helpful in noticing any cuts or wounds that have developed on the feet. Diabetes can produce tingling and numbing sensations in the feet. This may cause difficulty in feeling any cuts that are present on the feet, which can lead to infections. If the cuts are not properly cared for, foot ulcers may develop and gangrene may gradually develop. If you have diabetes, it is advised that you be under the care of a podiatrist who can manage this condition.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Milos Tomich, DPM from Dr. Tomich Foot & Ankle Health Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact one of our offices located in Milwaukee and Wauwatosa, WI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetic Foot Care
Diabetes can cause two problems that can potentially affect the feet: Diabetic neuropathy and Peripheral Vascular Disease. Diabetic neuropathy occurs when nerves in your legs and feet become damaged, which prevents you from feeling heat, cold, or pain. The problem with diabetic neuropathy is that a cut or sore on the foot may go unnoticed and the cut may eventually become infected. This condition is also a main cause of foot ulcers. Additionally, Peripheral vascular disease also affects blood flow in the body. Poor blood flow will cause sores and cuts to take longer to heal. Infections that don’t heal do to poor blood flow can potentially cause ulcers or gangrene.
There are certain foot problems that are more commonly found in people with diabetes such as Athlete’s foot, calluses, corns, blisters, bunions, foot ulcers, ingrown toenails, and plantar warts. These conditions can lead to infection and serious complications such as amputation. Fortunately, proper foot care can help prevent these foot problems before they progress into more serious complications.
Each day you should wash your feet in warm water with a mild soap. When you finish washing your feet, dry them carefully especially between your toes. You should also perform daily foot inspections to ensure you don’t have any redness, blisters, or calluses. Furthermore, if you are diabetic, you should always wear closed-toed shoes or slippers to protect your feet. Practicing these tips will help ensure that your feet are kept healthy and away from infection.
If you have diabetes, contact your podiatrist if you have any of the following symptoms on your feet: changes in skin color, corns or calluses, open sores that are slow to heal, unusual and persistent odor, or changes in skin temperature. Your podiatrist will do a thorough examination of your feet to help treat these problematic conditions.
Pregnancy and Foot Health
Many pregnant women complain about foot pain while they are expecting. Foot pain can primarily be caused by weight gain and hormonal changes taking place in the body. By understanding how pregnancy impacts the health of a woman's feet, a pregnant woman can take action to keep her feet as healthy and comfortable as possible.
Because a woman's weight changes during pregnancy, more pressure is brought to bear on both the legs and the feet. This weight shift can cause two major foot problems: over-pronation, also known as flat feet, as well as edema, which is swelling of the feet. Over-pronation occurs when the arch of the foot flattens, causing the foot to roll inwards when the individual is walking, and can aggravate the plantar fascia tissues located along the bottom of the feet. If these tissues become inflamed, a pregnant woman can experience pain in the heel of the foot as well as severe foot pain while walking or standing. Swelling of the feet, or edema, often occurs in the later stages of pregnancy. It is caused by slow circulation and water retention, and may turn the feet a light purple color.
To keep feet in good health and prevent over-pronation, pregnant women should avoid walking barefoot and be sure they are wearing shoes that offer good arch support. A device known as an orthotic can be added to regular footwear in order to provide additional support for the feet during pregnancy. Any expectant mother whose feet hurt should first check to see if the shoes she is wearing are old, worn out and not offering the proper support necessary for distributing the weight of her body during pregnancy.
To treat edema of the feet, a good start is to wear quality footwear which offers support and good circulation. Keep feet elevated whenever possible by using a foot stool while seated. Stay well hydrated by drinking plenty of water to prevent water retention in the feet. Any swelling that occurs in only one foot should be examined as soon as possible by a doctor.
Good foot health during pregnancy can help expectant mothers avoid foot pain that leads to other health problems. Massaging the feet and doing regular gentle exercise like walking aids foot health by contributing to good circulation. Supportive shoes are also a good investment that will support foot health during pregnancy.
Possible Causes Of Cracked Heels
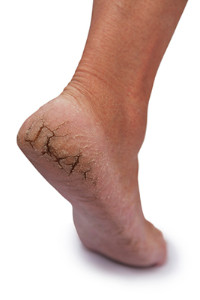 Cracked heels are a common foot condition, especially during the summer months. This can be a result of wearing shoes that have an open back, which typically provides inadequate support for the heel of the foot. The skin can become dry, and deep cracks that are known as fissures may form. Additional reasons why this condition may develop can include standing for extended periods of time throughout the day, excess weight the heels endure from being obese, and walking with a specific gait. Mild relief can be found when the feet are soaked in warm water, followed by using a good moisturizer frequently during the day. Research has indicated the importance of wearing shoes that fit properly, as this can be helpful in preventing cracked heels. If you are suffering from this ailment, it is suggested to consult with a podiatrist who can guide you toward the correct treatment.
Cracked heels are a common foot condition, especially during the summer months. This can be a result of wearing shoes that have an open back, which typically provides inadequate support for the heel of the foot. The skin can become dry, and deep cracks that are known as fissures may form. Additional reasons why this condition may develop can include standing for extended periods of time throughout the day, excess weight the heels endure from being obese, and walking with a specific gait. Mild relief can be found when the feet are soaked in warm water, followed by using a good moisturizer frequently during the day. Research has indicated the importance of wearing shoes that fit properly, as this can be helpful in preventing cracked heels. If you are suffering from this ailment, it is suggested to consult with a podiatrist who can guide you toward the correct treatment.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact Milos Tomich, DPM from Dr. Tomich Foot & Ankle Health Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact one of our offices located in Milwaukee and Wauwatosa, WI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How to Prevent Running Injuries
Overtraining and overusing the feet are the main causes of common running injuries. A number of these common injuries are caused by overrunning. Runner’s knee is a condition that is characterized by the back of the kneecap beginning to wear away and cause pain in the knee. This frequently occurs due to either a decrease in strength in the quadriceps muscles or ill-fitting shoes that are lacking in proper support for the inside of the forefoot. Strengthening exercises focusing on the quad muscle and sports orthotics are the usual treatments for those suffering from runner’s knee. Prevention of the condition lies in a focus on hip strengthening and quad-strengthening to keep the kneecap aligned. To help learn the best exercise to heal runner’s knee, one can also undergo physical therapy.
One common injury, called iliotibial band syndrome, is often caused by overtraining. This condition occurs when the iliotibial band gets irritated, creating pain and discomfort in the outside knee area. Plantar fasciitis, another common running injury, also occurs as a result of inflammation and irritation. Plantar fasciitis is an inflammation and irritation of the bone in the foot. A large amount of pain is often experienced due to plantar fasciitis. The condition can be caused by a high arch, improper footwear, tight muscles, or flat feet. It can best be avoided by stretching and wearing appropriate footwear that supports the foot.
Another common injury for runners is stress fractures. These injuries occur due to running style, overtraining, or a lack of calcium. Stress fractures most often occur in several locations in runners, including the inner bone of the leg, the thighbone, the bone at the base of the spine and the bones of the toes. Stress fractures are best prevented by wearing proper footwear and by running on flat and hard surfaces; this will absorb some of the shock created during running.
Aside from overtraining, other causes of common running injuries include ill-fitting footwear, a lack of flexibility and strength, and irregular biomechanics. The best way to avoid running injuries is to prevent them from even occurring. Both iliotibial band syndrome and stress fractures are preventable. The first step that should be taken to prevent running injuries is to only wear footwear that fits properly and that is appropriate for whatever activity you are doing. Running shoes are the only protective gear available to runners that can safeguard them from sustaining injuries. Choosing the right pair of shoes is therefore extremely important. While running shoes are an important factor, it is also important to consider other facets of your running routine such as training schedules, flexibility, and strengthening. These elements should be considered and altered according to your running needs to best maximize your run and minimize the possibility of injury. Careful stretching before and after a run should also be considered to help prevent running injuries. Stretching muscles enables greater flexibility and a lesser chance of sustaining injury.
Methods on Maintaining Proper Foot Care
 When the feet are properly cared for on a daily basis, certain foot conditions may be prevented from occurring. Athlete’s foot may be avoided when the feet are washed and thoroughly dried daily, especially between the toes. When a good moisturizer is applied, it may help to prevent cracked heels from developing. The importance of trimming the toenails properly is necessary in possibly preventing the painful condition known as ingrown toenails. Additionally, the feet will feel more comfortable when the correct size shoe is worn, and this can be accomplished if shoes are tried on in the afternoon when the feet are their largest. If you would like additional information about how to maintain proper foot care, it is advised to seek the counsel of a podiatrist.
When the feet are properly cared for on a daily basis, certain foot conditions may be prevented from occurring. Athlete’s foot may be avoided when the feet are washed and thoroughly dried daily, especially between the toes. When a good moisturizer is applied, it may help to prevent cracked heels from developing. The importance of trimming the toenails properly is necessary in possibly preventing the painful condition known as ingrown toenails. Additionally, the feet will feel more comfortable when the correct size shoe is worn, and this can be accomplished if shoes are tried on in the afternoon when the feet are their largest. If you would like additional information about how to maintain proper foot care, it is advised to seek the counsel of a podiatrist.
Everyday foot care is very important to prevent infection and other foot ailments. If you need your feet checked, contact Milos Tomich, DPM from Dr. Tomich Foot & Ankle Health Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Everyday Foot Care
Often, people take care of their bodies, face and hair more so than they do for their feet. But the feet are a very important aspect of our bodies, and one that we should pay more attention to. Without our feet, we would not be able to perform most daily tasks.
It is best to check your feet regularly to make sure there are no new bruises or cuts that you may not have noticed before. For dry feet, moisturizer can easily be a remedy and can be applied as often as necessary to the affected areas. Wearing shoes that fit well can also help you maintain good foot health, as well as making it easier to walk and do daily activities without the stress or pain of ill-fitting shoes, high heels, or even flip flops. Wearing clean socks with closed shoes is important to ensure that sweat and bacteria do not accumulate within the shoe. Clean socks help to prevent Athlete’s foot, fungi problems, bad odors, and can absorb sweat.
If you have any questions please feel free to contact one of our offices located in Milwaukee and Wauwatosa, WI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Types of Orthotics
 Orthotics are prescribed shoe inserts that can correct biomechanical foot issues. A podiatrist can evaluate your foot to see if a customized orthotic device is necessary, or if a standard shoe insert will suffice. Should you need orthotics, there are two different kinds. One type is rigid orthotics, otherwise known as functional orthotics. They are typically made from a material such as plastic, and are used in shoes with low heels in order to ease foot strain. The other type is soft orthotics, also known as accommodative orthotics. These provide a soft cushioning to help with issues such as plantar fasciitis or diabetic foot ulcers. These orthotics are bulky, so a special type of shoe may be required. Orthotics are typically more expensive than shoe inserts, but may last longer as they are made specifically for you. If you believe you may benefit from orthotics, or would like more information, you should consult with a podiatrist.
Orthotics are prescribed shoe inserts that can correct biomechanical foot issues. A podiatrist can evaluate your foot to see if a customized orthotic device is necessary, or if a standard shoe insert will suffice. Should you need orthotics, there are two different kinds. One type is rigid orthotics, otherwise known as functional orthotics. They are typically made from a material such as plastic, and are used in shoes with low heels in order to ease foot strain. The other type is soft orthotics, also known as accommodative orthotics. These provide a soft cushioning to help with issues such as plantar fasciitis or diabetic foot ulcers. These orthotics are bulky, so a special type of shoe may be required. Orthotics are typically more expensive than shoe inserts, but may last longer as they are made specifically for you. If you believe you may benefit from orthotics, or would like more information, you should consult with a podiatrist.
If you are having discomfort in your feet and would like to try orthotics, contact Milos Tomich, DPM from Dr. Tomich Foot & Ankle Health Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Are Orthotics?
Orthotics are inserts you can place into your shoes to help with a variety of foot problems such as flat feet or foot pain. Orthotics provide relief and comfort for minor foot and heel pain but can’t correct serious biomechanical problems in your feet.
Over-the-Counter Inserts
Orthotics come in a wide variety of over-the-counter inserts that are used to treat foot pain, heel pain, and minor problems. For example, arch supports can be inserted into your shoes to help correct overarched or flat feet, while gel insoles are often used because they provide comfort and relief from foot and heel pain by alleviating pressure.
Prescription Orthotics
If over-the-counter inserts don’t work for you or if you have a more severe foot concern, it is possible to have your podiatrist prescribe custom orthotics. These high-quality inserts are designed to treat problems such as abnormal motion, plantar fasciitis, and severe forms of heel pain. They can even be used to help patients suffering from diabetes by treating foot ulcers and painful calluses and are usually molded to your feet individually, which allows them to provide full support and comfort.
If you are experiencing minor to severe foot or heel pain, it’s recommended to speak with your podiatrist about the possibilities of using orthotics. A podiatrist can determine which type of orthotic is right for you and allow you to take the first steps towards being pain-free.
If you have any questions please contact one of our offices located in Milwaukee and Wauwatosa, WI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Ankle Sprains
Although ankle sprains may not be as serious as a broken ankle, they should be given immediate attention and care. An ankle sprain can lead to a significant amount of pain, as well as limited mobility. They are often characterized by the swelling and discoloration of the skin. This occurs when the ligaments are stretched beyond their limits.
The simple act of walking can sometimes cause a sprain, which makes ankle sprains a very common injury that can happen to anyone. They occur when the ankle twists in an awkward way or rolls over itself, causing a pop or snap in the tendons around the ankle. Some people are more at risk than others. These include athletes who continually push their bodies to the limits and also people who have previously suffered accidents to the feet, ankles, or lower legs.
Most of the time, an ankle sprain is not severe enough for hospital attention. There are many at-home treatment options available, including propping the leg up above your head to reduce blood flow and inflammation, applying ice packs to the affected area as needed, taking over-the-counter pain relievers and anti-inflammatory medication, using an ACE bandage to wrap and support the injured ankle, and most importantly, remaining off your feet until the ankle has fully healed.
Despite this, an ankle sprain can turn into a severe injury that might require hospitalization. If the ankle ligaments or muscles are damaged from a tear or rip, that is one sign that the sprain is severe enough for hospital attention and possibly for surgery. Even after the surgery, the recovery process can be long. You may need to have rehabilitation sessions administered by your podiatrist to get your ankle back to full health.
The severity of your sprain might become apparent if you are unable to stand or walk, consistent pain occurs over a prolonged period of time, swelling is much more severe than initially present, or if you start to experience tingling or numbness. These signs may indicate that your ankle sprain might actually be a broken ankle, an injury that requires immediate medical attention.
Although they are not completely avoidable, ankle sprains can be curbed with some preventative treatment measures. These include wearing appropriate-fitting shoes that not only provide a comfortable fit, but also ankle support. It is also recommended to stretch before doing any kind of physical activity, as this will help lower your body’s chance for an injury.